Melanoma is a type of skin cancer that originates from the pigment producing cells of the skin. Melanoma is the least common but also most dangerous type of skin cancer. It is usually seen on sun exposed areas like the legs or back, but it can also be seen in non-sun exposed areas and can occur anywhere on the body. Melanoma often appears like a new mole or it can begin from an existing mole. If left untreated, melanoma will grow deep into the skin and has the potential to spread to other parts of the body and become fatal. If detected early it is almost always curable.
Risk Factors:
- Having a history of intense intermittent sun exposure
- Blistering sunburns during childhood
- Fair skin and light eyes
- Increasing age
- A family history of melanoma in a first degree relative
- Inheriting certain genetic mutations
- Having multiple moles
- Having a history of atypical moles
- Tanning bed use
- Taking medications or having a condition that suppresses the immune system
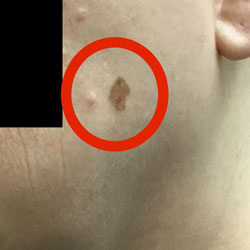
Signs and Symptoms:
- Will usually appear as a new or changing pigmented flat spot or bump
- Most melanomas are black or brown but it can also appear as skin colored or pink
- An existing mole that displays the ABCDE’s
- Asymmetrical: one half doesn’t match the other
- Border: irregular or uneven
- Color: a variety of colors present
- Diameter: larger than a pencil eraser (1/4 inch)
- Evolution: any mole that is changing in size, shape, or color or becomes elevated or symptomatic
- A mole that is an outlier and doesn’t look like the rest (the ugly duckling sign)
Diagnosis
- If Melanoma is suspected a prompt biopsy of the entire lesion should be performed and examined under the microscope by a dermatopathologist
- Depending on the depth of the lesion, additional testing may be required to diagnose the extent of the melanoma, such as a sentinel lymph node biopsy, MRI, CT, or PET scan.
Treatment
- Melanoma treatment is determined based on how deep it has penetrated into the skin and if any high risk features are seen under the microscope at the time of diagnosis.
- Melanoma on the surface of the skin, or in situ, is treated with Mohs surgery or surgical excision and the resulting wound sutured.
- Thin melanomas (less than 0.8mm) are removed with wide surgical excision and the resulting wound sutured.
- Thicker Melanomas (greater than 0.8mm) are also treated with wide surgical excision and the resulting wound sutured. However, further testing is usually done at this thickness.
- Sentinel Lymph Node Biopsy (SLNB) is considered for melanomas that are 0.8-1 mm deep and recommended for melanomas over 1 mm deep to determine if the Melanoma has spread internally. A radioactive substance or dye is injected near the Melanoma and a surgeon will then explore for the radioactive substance or lymph nodes stained with dye. If any lymph nodes are identified they are removed and examined for the presence of any cancerous cells. If a SLNB is positive for cancerous cells, a more aggressive treatment plan will usually be required in addition to surgical removal of the m
- Additional treatment for melanoma that has metastasized can include radiation therapy, chemotherapy, or immunotherapy.
Course and Prognosis:
- Melanoma accounts for about 1% of all skin cancers but causes the most skin cancer deaths. When found early, melanoma can often be cured with surgery.
- If left untreated, melanoma will grow further into the skin and spread to nearby organs and lymph nodes. When this happens it is considered advanced and the survival rate is fair to poor.
- In-situ melanomas have an excellent prognosis with surgical removal/Mohs and there is no risk of spread beyond the skin.
- Thin Melanomas have a very good prognosis with early diagnosis and treatment and very low risk of recurrence and metastasis.
- Intermediate thickness Melanomas with high risk features and thick melanomas are at a high risk of metastasizing to nearby lymph nodes.
- The 5 year survival rate for thin melanomas is around 97%, 63% once it has spread to nearby lymph nodes, and 20% once it has spread internally to organs.
- Once a Melanoma has been diagnosed, a full body skin exam should be performed every 3-6 months for 2-3 years, and then yearly after that.

